Home / DEPARTMENTS / Interventional Radiology
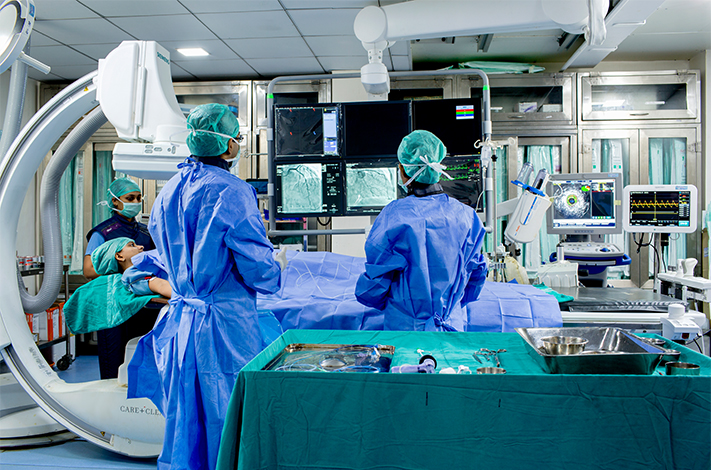
What is interventional radiology?
Interventional radiology (IR) is a sub-specialty of radiology that has become increasingly important since the mid-1970s, contributing to some of the most significant medical developments in recent years. Under image guidance (x ray or sonography) interventional radiologist enters blood vessel of body via small cut on skin and can provided treatment of variety of disease locally by using special tubes (catheters), wire, stent or blocking agents. It also includes non-vascular procedures like biopsy, drainage of infected fluid collection in body.
What are the advantages of interventional Radiology?
It has significantly lower amount of risk, less pain (as large incision are not required), shorter recovery time and minimal hospital stay compared to conventional surgical procedures. Most of the procedures do not require having a general anesthesia.
Department of Interventional Radiology (IR) at Medical Trust Hospital is capable of doing all kind of interventional procedures for entire body. It may be opening of blood vessel in brain, neck, abdomen, legs to blocking of abnormal blood vessels to treat liver cancer, fibroid, bleeding in stomach etc. IR procedures can be used in almost every organ system, and the list of conditions that can be diagnosed and treated using image-guided techniques is continuously growing. Department also offers 24 x 7 hours service for acute stroke (paralysis) patient to remove clot from blood vessel of brain (mechanical thrombectomy).
- Vascular Intervention
- interventional radiology is the mainstay of treatment in cases of haemorrhage from GI tract, hemoptysis, epistaxis, hematuria, antepartum and postpartum haemorrhage.
- An angiogram is done to determine the cause of bleed
- The usual lesions can be embolised with coils, Abgel or polyvinyl alcohol particles
- Angioplasty and stenting can be done for peripheral vessels which are stenotic or occluded. Patients get a new lease on life because many limbs can be saved from unnecessary amputations or the extent of amputation can be limited. There is relief from claudication pain, rest pain and ulcer healing are fascinated.
- Time is Brain – One of the most miraculous moments in modern medicine is to open up a blocked vessel early enough, when the damage has not yet been severe, and then restore the blood flow and watch the incapacitated stroke patient return to a completely normal state. Timely intervention in stroke patients with thrombolysis and clot aspiration can prevent significant post stroke morbidity. Intra-arterial thrombolysis and mechanical removal of clot can be done if patient presents within 6 hours of stroke onset.
- Renal artery stenosis can be corrected in patients with renal hypertension
- Repair of dialysis fistula stenosis/occlusion
- Interventional radiology is the treatment of choice in arteriovenous malformations. The feeder vessels are cannulated with microcatheters and the lesion is embolised with glue or absolute alcohol
- Coiling of cerebral aneurysms is safe and effective without the attendant morbidity of surgery
- Traumatic pseudoaneurysms can be treated by coiling or stent graphics
- Aortic aneurysms and dissections are corrected
- Embolisation of the feeders of the fibroid can be done leading to shrinkage in the size of the fibroid. The procedure has less morbidity than a surgical procedure with reduced hospital stay. This is especially useful in patients who are high risk for surgery.
- Embolisation of tumors prior to surgery significantly reduces preoperative bleeding especially in cases of juvenile nasopharyngeal angiofibromas, bone tumours and renal tumours
- This is useful in intermediate stage hepatocellular carcinoma
- Adriamycin is injected directly into the tumour bed along with polyvinyl alcohol particles. The combined effects of schemia and chemotherapy help in tumour regression
- Acute limb ischemia is one of the commonest vascular emergencies. Injection thrombolytic agents in the clot aspiration can save the limb
- Injection of sclerosant into venous malformations cause them to shrink in size
- The procedure is done under ultrasound or fluoro guidance. It is a simple and safe procedure.
- The lesions cannot be cured but there is significant size reduction and symptomatic relief.
- Treatment of varicose veins using laser technology. The vein is accessed with a needle. The laser fiber is introduced in to the vein and activated.
- On withdrawing the fiber the vein gets occluded.
- This is an outpatient procedure.
- A significant number of people suffer from chronic venous insufficiency following DVT. Their quality of life can be improved with timely intervention.
- The thrombus in the vessel can be aspirated and lysed with rtpa or urokinase if the patient presents within 2 weeks of onset of DVT.
- Patients suffering from intractable ascites or recurrent episodes of hematemesis benefit from percutaneous portosystemic shunting procedure.
Vascular intervention can be broadly divided into arterial and venous interventions
Arterial Interventions
1) HAEMORRHAGE
Vascular intervention is a safe and effective way of controlling bleeding especially because surgical treatment has high morbidity in such a scenario and many lesions are not accessible surgically.
2) REVASCULARISATION
3) AVM
4) UTERINE FIBROID EMBOLISATION
5) PREOPERATIVE EMBOLISATIONS
6) TRANSARTERIAL CHEMOEMBOLISATION
7) INTRAARTERIAL THROMBOLYSIS
Venous Interventions
1) SCLEROTHERAPY
2) ENDOVENOUS LASER THERAPY FOR VARICOSE VEINS
3) DVT
4) TIPPS
- Non Vascular Interventions
- Percutaneous Vertebroplasty
- Percutaneous Drainages including Percutaneous Nephrostomy and Biliary Drainage, Oesophageal Stenting
- CT/USG guided FNAC's, biopsies
- Neuro Procedures
- Brain aneurysm- coiling, balloon assisted coiling, stent assisted coiling, flow diverter
- Acute stroke interventions – mechanical thrombectomy
- Venous sinus thrombosis – in situ thrombolysis.
- Brain AVM/AVF embolization
- Dural AVF embolization
- Carotid artery stenting
- Intracranial stenting
- Vein of Galen malformation embolization
- Spine
- Spine and spinal cord vascular malformations
- Spinal Dural AV fistula
- Spine and spinal cord hyper vascular tumors Embolization
- Vertebroplasty
- ENT
- Embolization of hyper vascular tumors (Angiofibroma, paraganglioma, carotid body tumors)
- Maxillofacial vascular malformation
- Percutaneous sclerotherapy of venous / lymphatic malformation /hemangioma
- Epistaxis
- Neck aneurysms
- Traumatic vascular injuries
- Oncology
- Transarterial chemoembolization for liver cancer
- RF ablation of tumors
- Pre-operative tumor embolization
- Percutaneous gastrostomy
- Emergency - Life Saving
- Post traumatic bleeding
- Post-surgery/post biopsy bleeding
- GI bleeding
- Massive hemoptysis
- Acute limb ischemia – thrombolysis
- Gynecology And Obstetrics
- Embolization of fibroid
- Post partum hemorrhage embolization
- Uterine AV malformation embolization
- Fallopian recanalization
- Urology And Nephrology
- Permanent hemodialysis catheter insertion
- Dialysis AVF salvage
- Renal biopsy percutaneous or trans-jugular
- Post biopsy bleeding – embolization
- PCN
- Hepato Biliary
- TIPS Transjugular Intrahepatic Portosystemic Shunt
- DIPS- Direct Intrahepatic Portosystemic Shunt
- BRTO Balloon Occluded Retrograde Transvenous Obliteration of gastric varices
- PTBD- Percutaneous Transhepatic Biliary Drainage
- Budd chiari syndrome - hepatic vein/IVC stenting
- Biliary stenting
- Trans-jugular liver biopsy
- Portal vein embolization
- Arterial Diseases
- Angioplasty and stenting of peripheral arteries
- Renal artery stenting
- Mesenteric stenting
- Aneurysm – embolization/ stent graft
- AORTA
- Aortic aneurysm - stent graft
- Aortic dissection - stent graft
- Traumatic aortic injury
- Aortic stenosis / Aorta-arteritis
- Venous Interventions
- IVC Filters
- Thrombolysis in DVT
- Varicose vein – RF / LASER ablation and foam sclerotherapy
- Congenital Vascular Malformation
- AVM / AVF embolization
- Percutaneous sclerotherapy for venous & lymphatic malformation
- Carbon Dioxide (CO2) Angiography for renal impaired patients



